Undiagnosed diseases: definition, statistics, problems and solutions
A new decade begins. In Quebec, we are hopeful that by 2020, action will finally be taken to improve the health and living conditions of people with rare and orphan diseases, as well as their caregivers and families. It will have taken a decade of awareness-raising, education and advocacy on the part of the Regroupement québécois des maladies orphelines(see initiatives here) and other players for the Quebec government to finally catch up with other industrialized countries. We hope that the same will be true for the rest of Canada, so that all rare disease sufferers will be less orphaned by their respective provincial health systems and research programs.
People with rare and undiagnosed diseases
Can we call them zebras? Because technically zebras are rare diseases known from common diseases (horses). Swans? There are a number of organizations around the world dedicated to helping the undiagnosed. They are known by the acronym SWAN. SWAN stands for Syndromes Without A Name. There’s SWAN UK, SWAN Australia, SWAN USA.
Unless you’re very creative, it’s hard to use “swan” as a French acronym for “Syndromes sans nom”. SNN? Why not “Syndrome sans diagnostic fixe”? SSDF, like itinérants or SDF, “Sans domicile fixe”, because without a fixed diagnosis, you don’t have a fixed address in the healthcare network, and without a name and address, it’s hard to get services.
We can distinguish two groups of people without a diagnosis:
- The ” not yet diagnosed“These are patients who may have a known rare disease, but who have not been referred to the appropriate service for diagnosis, or who have an unusual clinical presentation of the disease, or who have common non-specific symptoms that are misleading. It is hoped that they will eventually be diagnosed, and this may take some time.
- The ” undiagnosed“These are patients for whom every effort has been made to obtain a diagnosis, but who suffer from a disease that has not yet been characterized and is therefore not a known rare disease. We’ve exhausted the tests and examinations available, and we still don’t have an answer. Some people obtain a diagnosis thanks to the use of new tests (for example, in genetic research using exomic or genomic DNA sequencing).
We could also define a third category: people with an ” ambiguous diagnosis “. They either have a diagnosis of “probable known disease X” or “atypical disease X”, or there is some hesitation between disease X and disease Y.
The diagnostic odyssey
All these people go through a period of diagnostic wandering of varying lengths (their whole lives for some), which may be interspersed with false diagnoses or, failing a diagnosis of a physically caused illness, a psychiatric diagnosis.
How long does it take to diagnose a rare disease?
According to the survey conducted in Quebec by RQMO in 2010 (answered by nearly 300 patients or caregivers):
- for 37% of respondents, it took 3 years or more to obtain their diagnosis;
- for 27% of respondents, it took 5 years or more;
- for 18% of respondents, it took more than 10 years;
- 30% consulted 5 or more doctors before obtaining their diagnosis.
(Please note: The diseases diagnosed were all known rare diseases)
Testimonial from the survey :
I had to wait 30 years for a diagnosis. My medical care is scattered all over the place through various specialists, most of whom don’t know what disease I have and only treat the symptoms without really understanding what I have. Everything I know about my illness I know because I’ve read up on it over the years on the internet; very few doctors have given me answers and many have given me false information about it. It’s also very difficult to find specialists or paramedics like physiotherapists who know about the disease and can treat me in the right way. .
Other data from a Canada-wide survey conducted by the Canadian Organization for Rare Disorders (CORD) and answered by over 500 people in 2014.
- for 22% of respondents, diagnosis took 3 to 12 months;
- for 17%, from 3 to 6 years old;
- for 24%, more than 6 years.
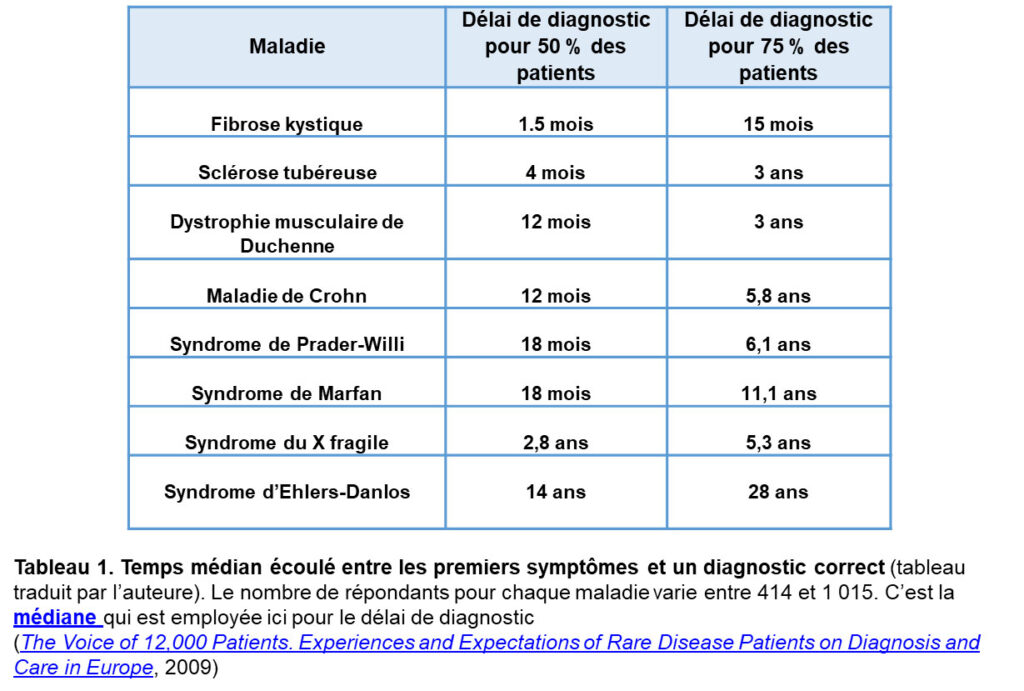
And here we present a table taken from a Eurordis survey of 12,000 patients in Europe (The Voice of 12,000 Patients. Experiences and Expectations of Rare Disease Patients on Diagnosis and Care in Europe , 2009):
Table 1. Median time from first symptoms to correct diagnosis (translated by the author). The number of respondents for each disease ranged from 414 to 1,015. The median is used here for time to diagnosis.
Click on picture to enlarge
Many obstacles encountered during the diagnostic wandering period :
- Incredulous doctors faced with “bizarre” symptoms or a common set of non-specific symptoms, leading them to consider a psychiatric diagnosis.
- Victims of “front-page syndrome “*, i.e. the inclusion in medical records of a reference to a psychological problem, a psychosomatic condition or a psychiatric illness (* expression used by health lawyer Jean-Pierre Ménard).
- Stigmatization of patients for consulting numerous doctors (“they store around”).
- GPs discouraged by their inability to diagnose and treat.
- Patients who question their own mental health.
- Treatment of symptoms by trial and error.
- Unnecessary or inappropriate surgery.
- Unanswered questions about the possible hereditary transmission of the disease and the likelihood of another family member being affected.
- Difficulty accessing services or programs even when there are real handicaps or disabilities (financial assistance programs for the handicapped or disabled, rehabilitation centers, reimbursement for medical equipment, programs in the workplace or at school, etc.).
- And, last but not least, there is often a lack of understanding on the part of those around them of the patients’ or parents’ quest to find a name and an explanation for their illness or that of their child.
How many people are ill without a diagnosis?
We often read or hear that “40-50%” of patients are undiagnosed. This statistic is presented without any bibliographical source. It may be a dated figure that still persists in the literature on rare diseases, as there are few accurate statistics in the field of rare diseases. Perhaps it refers to diseases or syndromes often found in paediatric wards? In days gone by, perhaps one out of every two sick children had a malformative syndrome, with or without intellectual disability, and had not been diagnosed.
In Japan, an attempt was made to estimate the number of “undiagnosed” patients. The study concluded that there were over 37,000 undiagnosed patients in the Japanese healthcare system. The total population of Japan is 127 million. The number of people with rare diseases in Japan can be estimated at around 6 million. A number of 37,000 undiagnosed patients seems low, but we have few points of reference.
(Reference : Survey on patients with undiagnosed diseases in Japan: potential patient numbers benefiting from Japan’s initiative on rare and undiagnosed diseases (IRUD), Takeya Adachi and colleagues, Orphanet Journal of Rare Diseases. 2018. 13: 208.)
Although it’s difficult to say how many “undiagnosed” patients there are in Quebec or elsewhere, today, the success rate of diagnosis has increased following the characterization of thousands of syndromes, the development of diagnostic tools, advances in genetic technology (exomic, genomic and RNA high-throughput sequencing) and the more rapid sharing of knowledge. We dare to hope that there are now fewer than 40-50% of undiagnosed patients.
What can be done to reduce diagnosis times for rare diseases?
In 2016, an international coalition of patient organizations published five recommendations to address the specific needs of rare patients without a diagnosis:
- Patients with undiagnosed rare diseases should be recognized as a distinct population.
- Every country should have sustainable national programs dedicated to people without a diagnosis.
- Knowledge and information sharing should be structured and coordinated at national and international level.
- Patients should be involved in the governance of these programs to set priorities.
- Promote ethical and responsible data sharing.
(Source: International Recommendations to Address Specific Needs of Undiagnosed Rare Disease Patients)
Proposals to reduce diagnostic delays in Quebec
In the Quebec strategy for rare diseases drafted by RQMO following numerous consultations, here are the proposals put forward to reduce diagnosis delays in Quebec:
- Training of future doctors and continuing education on existing tools and resources for diagnosing rare diseases, and on the approach to take with the patient if a diagnosis cannot be found.
- Register of medical experts in certain rare diseases by specialty.
- Establish rare disease clinics by specialty (centers of reference).
- Establish clinics or programs dedicated to patients with undiagnosed diseases
- Use of telemedicine
Particularly for diseases of genetic origin:
- Better training of doctors to identify hereditary diseases in families or signs/diagnoses that increase the risk of having a child with a genetic disorder
- Increase and organize medical genetics resources to free up medical geneticists for more diagnostic work (more genetic counselors).
- Outreach genetic clinics in the regions of Quebec (with genetic physicians and genetic counselors).
- Standardize genetic testing across medical genetics and other services (neurology, hereditary cancer clinics, etc.).
- Establish one or more genomics centers to offer high-throughput sequencing for clinical diagnostic purposes (not just for research, and for both adults and children).
- Develop preconception, prenatal and neonatal screening programs
- Develop screening programs for certain categories of disease (e.g. hereditary cancers, immunodeficiencies, etc.).
January 19, 2020, Gail Ouellette, Regroupement québécois des maladies orphelines
Updated July 2023:
- See the MSSS’s Politique and Plan d’action québécois pour les maladies rares, published in 2022 and 2023, respectively.
- See RQMO’s 2022 Annual Education Day on the theme of diagnostic wandering.